Addiction recovery is hard. People struggling with addiction need lots of help and support. Telemedicine offers a novel approach to receiving help from the comfort of home. This method utilizes technology to connect patients with healthcare providers. Patients have the option to access addiction treatment via video calls, phone calls, text messaging, and specialized applications.
- Telemedicine Helps More People Get Treatment
- Finding the Right Telemedicine Provider
- Different Types of Telemedicine for Addiction
- Research Shows Telemedicine Improves Addiction Treatment
- Telemedicine Myths and Facts
- Important Rules Protect Patients
- Challenges and Limits of Telemedicine
- Exciting Improvements Coming Soon
- Patients Are Happy with Telemedicine
- One Patient’s Recovery Story
- Conclusion
- Frequently Asked Questions
Telemedicine Helps More People Get Treatment
In-person treatment can be difficult. Many people live far from addiction centers. Some people don’t have cars or can’t drive. Some people have disabilities making travel hard. Numerous individuals prefer to maintain privacy regarding their addiction from family members or employers.
Telemedicine makes treatment easier to get. Patients don’t have to travel or take time off work. They can get help discreetly from home. Virtual care ensures that more people can receive expert support precisely when they need it the most.
Finding the Right Telemedicine Provider
Choosing the right telemedicine provider is key. Ensure that potential providers are licensed and employ proven treatment methods. Ask about their areas of specialty and addiction training. See what services they offer like counseling, group sessions, and apps. If paying without insurance, it’s important to compare costs. Read online reviews from past patients. Finding a compassionate, reputable provider like Ohio PHP sets the stage for success.
Different Types of Telemedicine for Addiction
There are two main types of telemedicine services:
Live Video Appointments
Patients can join virtual sessions like:
- Individual and group counseling
- Psychiatrist and doctor visits
- Family therapy
- 12-step meeting support groups
Seeing a therapist or counselor by video call is just like being in-person. But patients save time by not traveling.
Store-and-Forward Services
Other telemedicine options allow patients to access help at a pace that suits them:
- Educational videos and recovery messages to view whenever needed
- Self-help tools and exercises to build recovery skills
- Health tracking apps to monitor progress or triggers
- Prescription access and medicine reminders
New mobile apps also provide 24/7 support. Patients can use AI chatbots for quick questions. They can join online peer support groups or access emergency resources if they feel triggered or unsafe.
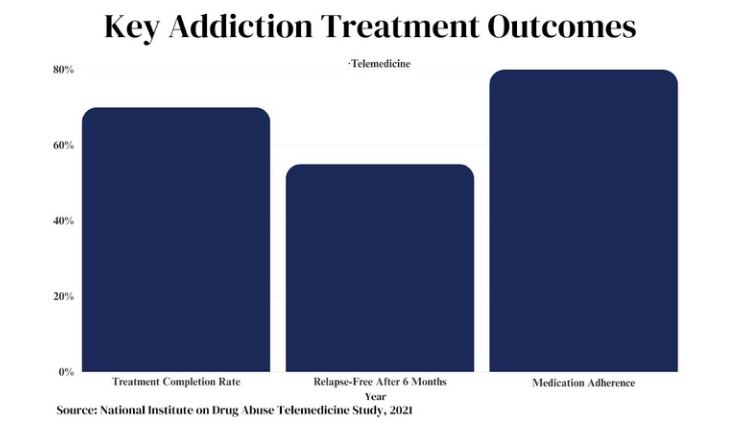
Research Shows Telemedicine Improves Addiction Treatment
Many studies prove telemedicine works well for addiction recovery. Patients achieve better outcomes compared to solely in-person treatment. Benefits include:
- Patients engage in treatment for longer periods
- Patients have fewer relapses after treatment
- Patients take medication properly and consistently
- Patients reduce dangerous drug-using behaviors
- Patients improve social and work functioning
Telemedicine is as effective as in-person care for many addictions. This includes alcohol, opioids, tobacco, and more.
Telemedicine Myths and Facts
Some common myths about telemedicine keep people from trying it. However, the facts demonstrate its considerable effectiveness:
Myth: Telemedicine is impersonal. Fact: Providers can build close therapeutic relationships remotely.
Myth: Remote treatment is lower quality. Fact: Telemedicine delivers equal results to in-person treatment.
Myth: It’s not private or secure. Fact: Strict laws protect telemedicine privacy like any healthcare.
Learning the truth behind telemedicine myths can make people feel confident choosing it.
Important Rules Protect Patients
Like all healthcare, telemedicine must follow ethical practices and protect privacy. Providers are required to comply with HIPAA laws regarding:
- Keeping patient information private and secure
- Requiring patient consent to share any records
- Safely handling and storing confidential data
Other considerations include:
- Licensing laws if providers treat patients in different states
- Prescription guidelines for controlled medications
- Documentation policies for informed consent
Challenges and Limits of Telemedicine
Telemedicine has many benefits but some challenges too:
- Technical problems like poor internet or video quality
- Harder for providers to build strong relationships remotely
- Physical exams and drug tests must be done from home
- Insurance does not always cover telemedicine treatment
Still, telemedicine removes enough barriers that treatment becomes accessible. This helps when in-person options are not possible for a patient.
Exciting Improvements Coming Soon
New technologies may expand telemedicine services even more. Possible advances include:
- Virtual reality tools for therapy and skills practice
- At-home patient monitoring devices
- Improved drug testing kits to use from home
- AI and data to personalize treatment plans
New state policies and insurance changes could also increase coverage. This would allow more patients to use telemedicine.
Patients Are Happy with Telemedicine
What do patients think about telemedicine for addiction treatment? Surveys show very high satisfaction:
- It is convenient and easy to access from anywhere
- It allows discreet and private care
- It provides flexibility to get help on a busy schedule
- Patients can keep attending work, school, or family duties
- Virtual care reduces travel time and costs
Many say telemedicine is key for their ongoing recovery success. They could not get adequate treatment without it.
One Patient’s Recovery Story
Sarah struggled with alcohol addiction for many years. Her busy job and long commute made in-person treatment hard. Whenever she tried, she would relapse within weeks.
After learning about telemedicine, Sarah decided to try it. She started with online counseling and took education courses. These taught new techniques to prevent relapse. She also used a recovery app and connected with a sponsor for daily check-ins.
Within months, Sarah put together days and weeks of sobriety. For the first time, she had the tools and support to maintain recovery at home.
Sarah’s story shows how telemedicine can empower successful addiction treatment. Removing barriers is the first step.
Conclusion
Getting help for addiction is not easy. But telemedicine gives new hope. It uses technology to bring treatment home. Patients can get support through phones, video chats, texts and apps.
Telemedicine breaks down barriers. Now more people can get the help they need. It saves them time and lets them keep treatment private. Patients don’t have to take off work or find childcare. They can attend counseling at night after kids sleep.
The research shows telemedicine helps patients stay sober longer. Relapses happen less often. Patients learn healthy skills for life at home. They can access therapy 24/7 instead of waiting for appointments.
Telemedicine isn’t perfect. But it makes treatment possible when people have no other options. Patients feel empowered taking control of their recovery. They have tools to fight this tough disease.
Addiction thrives in isolation. Telemedicine connects people to experts and peers. Having daily support keeps them on track. It gives them hope during the hard parts. Every patient deserves a chance at recovery. Telemedicine helps make it happen.
Frequently Asked Questions
What if I feel unsafe or have an emergency?
Tell your provider right away. Many offer 24/7 crisis resources. Get help from 911 or emergency rooms if needed.
Will telemedicine work if I have a job or family?
Yes, telemedicine is designed to be flexible around your schedule. Providers understand life responsibilities.
What happens after telemedicine treatment ends?
Your provider will help you transition to ongoing community supports. These maintain recovery success long-term.
How can family and friends support my telemedicine treatment?
Loved ones play a big role. Consider including them in counseling sessions. Ask them to help you stay accountable.




