Health Research Policy: where the world of medicine and health care is an ever-evolving landscape
Plantar Fasciitis Heel Pain Explained
Heel pain can disrupt your daily life, making even simple activities like walking or standing uncomfortable. Plantar fasciitis is one…
Why Leading Pathologists Choose NovoPath LIS for Enhanced Laboratory Efficiency
In today’s fast-changing healthcare environment, pathologists are under more pressure than ever to deliver precise, efficient, and quick disease diagnoses.…
How Hospitals Clean Medical Devices
Cleaning medical devices at a hospital isn’t quite the same as washing dishes or other everyday items at home. While…
Health Research News
Why Leading Pathologists Choose NovoPath LIS for Enhanced Laboratory Efficiency
In today’s fast-changing healthcare environment, pathologists are under more pressure than ever to deliver precise, efficient, and quick disease diagnoses. Tools like lab management software, specifically NovoPath, are disrupting the…
The Emerging Science of Molecular Hydrogen Therapy
In the evolving landscape of alternative therapies and health innovations, molecular hydrogen therapy is one of the most exciting developments. This innovative approach leverages the simplicity and abundance of hydrogen,…
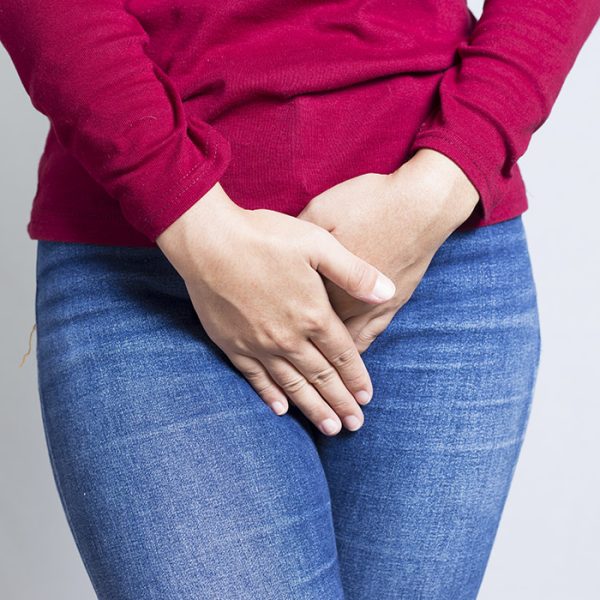
How to Restore Pelvic Floor Strength and Function
Restoring pelvic floor strength and function is an endeavor that holds transformative potential for one’s health and quality of life. This journey, often embarked upon in the aftermath of childbirth,…
Subscribe to our latest health news & articles
Personal Health
Transformative Strategies for Effective Addiction Recovery
Addiction is a formidable opponent, affecting millions of individuals worldwide. Whether it’s substance abuse, alcoholism, gambling, or any other form of addiction, the journey to recovery can be challenging and…
Eat, Move, Thrive: Holistic Health Guide
Forget the latest diet trend or punishing gym routine. True health, the kind that makes you feel energized and ready to tackle anything, comes from a more balanced approach. It’s…
Health Technology
Facts vs Fiction
Home And Healing: Recognizing When A Loved One Needs Mental Health Treatment With Housing
In the journey of life, our loved ones sometimes face challenges that go beyond their ability to cope with on their own. Mental health issues can be particularly debilitating, and…
The Importance of Hospital Textiles in Terms of Comfort, Hygiene, and Care
Patients may have difficult periods during their stays in the hospital; therefore, the importance of textiles such as gowns, sheets, blankets, and shower curtains cannot be overstated. The provision of…
Debunking 5 Myths About Going to Rehab for Substance Abuse
Going to rehab for substance abuse is a decision that can change your life, and it can be a scary prospect for many. Unfortunately, there are many myths and misconceptions…